
Over 50 million children suffer from acute malnutrition every year and 80 percent of them don’t have access to treatment. Many have to walk for miles in search of health services with no guarantee of receiving help once they arrive. Even if treatment is available, few children are able to continue it until they successfully regain their health.
These situations will only continue to worsen as conflict and violence overtake countries in need. One in thirteen children around the world are living in a war zone, where conflict can halt food production, close ports and destroy critical health services.
Last year, International Rescue Committee President and CEO David Miliband visited a malnutrition treatment centre in Nigeria, devastated by what he saw:
“Every bed in the centre was full, and when you spend time with the children who have just arrived, you see how close they are to death,” says Miliband. “Even more painful was knowing that for every child we could treat there were ten more children in need and unreached.”
Remember that malnutrition isn’t just hunger. It’s a life-threatening condition that can permanently impair development, increase the risk of infection and disease, and rob these children of the opportunity to live full, healthy and productive lives.
The world is in need of new solutions, and the IRC has developed several that together offer the potential for transformative change.
After four years of research and successful studies in Kenya and South Sudan done with partner organisations Action Against Hunger, No Wasted Lives, and the London School of Tropical Medicine and Hygiene, we’ve developed a game-changing approach to combat acute malnutrition.
“We have a clear and proven solution,” says Miliband. “It is possible to go from just 20 percent of children treated for acute malnutrition to 90 percent.”
Here’s how.
1. Create a unified treatment programme.
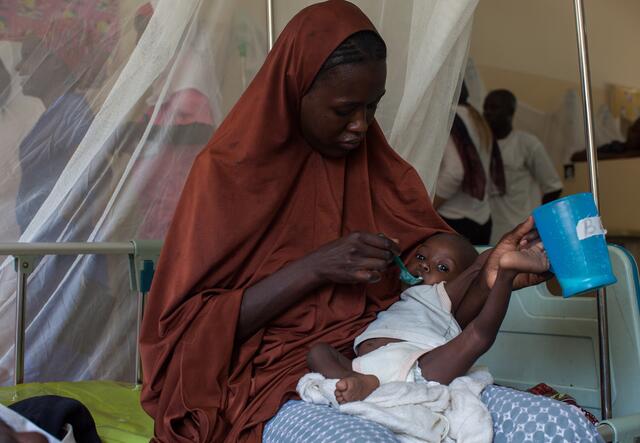
There are currently two different treatments for children with severe acute malnutrition and children with moderate acute malnutrition, supported by two different United Nations agencies. This duplication creates inefficiencies, wastes critical resources, and makes it difficult for children to access the care they need.
Since both treatments are rarely available at the same time, children with moderate acute malnutrition are often left to wait until they become more critically ill before receiving help. And when a child with severe acute malnutrition recovers but is still categorised as having moderate acute malnutrition, they may be referred to a different clinic for treatment, or treatment may be stopped altogether. This approach keeps these children caught in a vicious cycle. All too often their health backslides, putting them right back in the severe category, where their risk of death is nearly ten times higher than that of a healthy child.
The IRC believes the way forward is to create a combined and simplified treatment process—one that allows all children with acute malnutrition to be treated using a single programme. Our research, similar to other studies that have examined combined approaches to acute malnutrition treatment, found that it is effective to treat children with severe and moderate acute malnutrition together.
Going forward, this combined approach will allow humanitarian organisations and U.N. agencies to work closely together on delivering care that will save costs and, most important, save more lives.
This important work is already being carried out. In Mali, the IRC is able to treat children for malnutrition through this combined approach with support from the EU.
2. Bring treatment to children, instead of the other way around.
Currently families must bring sick children to a health facility for treatment. Such journeys are not only difficult when ill, but also impossible in many conflict-ridden countries. These treks can take hours on foot through extremely dangerous territory, or there may not be health facilities in reach. In countries like Yemen, health workers can’t even get to the facilities because they’re under attack.
Our solution is to bring treatment straight to the children in their homes and communities. We’ve already seen success with this approach in training health workers to treat diseases like pneumonia or malaria. In Ethiopia, trained workers are placed at health posts across the country, which has helped to reduce child mortality by two-thirds.
Sick children need treatment right when and where they need it.
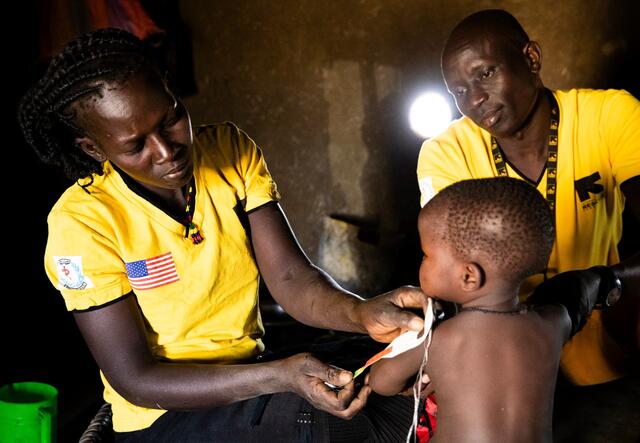
Sick children need treatment right when and where they need it. That’s why the IRC created simple and intuitive tools that community health workers can use to diagnose acute malnutrition. One example is a colour-coded armband that anyone can use to measure upper-arm circumference. We’ve also created scales with pictures illustrating the appropriate dose of therapeutic food for a child's size, to enable community health workers who may not be literate to not only diagnose but also treat acute malnutrition.
3. Scale up funding and the political will to save lives

Delivering care for acute malnutrition through a combined approach offers the promise of stretching every dollar for treatment further. But for lives the world over to truly be transformed, greater political will and funding are needed to reach every child who is suffering. Governments, policymakers and humanitarians around the globe can help ensure that these approaches are actually taken up, fully funded, and put into practice.
By scaling up this three-part solution, the IRC believes that we can help the over 50 million children suffering from acute malnutrition every year and save the lives of nearly a million children over the next decade. Learn more about our work.
Research findings update: July 10, 2020
Experts anticipate a rise in the number of malnourished children in 2020 as a result of food crises related to the COVID-19 pandemic. A new streamlined approach to treating acute malnutrition is as effective as standard treatment but will free up funds to reach more children with lifesaving care, according to new research published in PLOS Medicine. The study was led by the IRC, the London School of Hygiene & Tropical Medicine, and Action Against Hunger. Learn more.
With support from EU Humanitarian Aid, the International Rescue Committee is able to treat children for malnutrition in countries like Mali.

