
Around the world, an estimated 45 million children under the age of five experience acute malnutrition at any given time. Up to two million of these children die as a result annually.
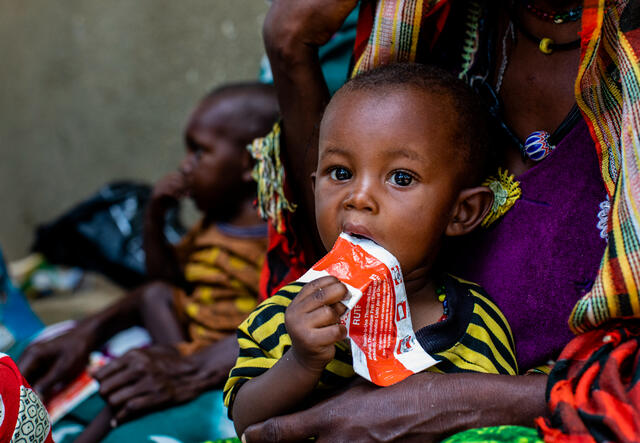
The surging global hunger crisis is dire, especially for vulnerable children who are at heightened risk. However, there is a promising solution: treatment with a high protein peanut paste known as ready-to-use therapeutic food (RUTF). This innovative intervention has demonstrated remarkable effectiveness in combating malnutrition, providing essential nutrients that help children recover and thrive. By ensuring access to RUTF, we can make significant strides in addressing the devastating impact of hunger and improving the lives of countless young individuals around the world.
More than 90 percent of malnourished children treated with RUTF recover within weeks. But this simple, effective and scalable solution is still out of reach for too many children. Historically, more than four of every five children with acute malnutrition do not receive this lifesaving treatment they need due to unnecessary, life-threatening bureaucracy and lack of sustained funding.
The International Rescue Committee (IRC) treats children experiencing acute malnutrition in 21 countries. Scaling up our approach and delivering these simplified, proven solutions will save lives.
Many complex global problems don’t have a simple solution, but this one does. Read on to learn more about acute malnutrition, why children aren’t receiving the treatment they need, and how we can build a world where no child dies of hunger.
What is acute malnutrition?
Children experiencing acute malnutrition are too thin for their height and as their bodies weaken from a lack of nutrition, they become more vulnerable to other diseases. They are 11 times more likely to die than healthy children.
Even if a child survives acute malnutrition, they often face long-lasting harmful effects from it. Acute malnutrition can negatively impact physical and mental development, especially in children under the age of five who are in a critical period of growth.
“This is a grim reality. The world cannot afford to stand back and watch,” says Elijah Okeyo, the IRC’s Uganda country director

What factors contribute to acute malnutrition?
In 2023, nearly 282 million people in 59 countries faced high levels of acute food insecurity, requiring urgent food and livelihood assistance.
Many countries with high rates of children experiencing acute malnutrition suffer disproportionately from the effects of climate change, which has increased the severity of droughts and floods, destroying food supplies and livelihoods. The growing global hunger and malnutrition crisis is directly linked to climate change. Climate shocks damage critical infrastructure, limiting access to clean water and sanitation. In such cases, diseases can spread rapidly – often among populations of children whose immune systems are already weakened by malnutrition.
Countries like Somalia, which endured three consecutive years of severe drought followed by flash flooding , are feeling the impacts firsthand. This continues to affect 4.3 million people who are facing crisis levels of food insecurity. The drought also decimated people’s livelihoods, especially those in the agro-pastoral sector, with over 3.5 million livestock having perished.
Conflict is also a driver of hunger and malnutrition because of the ways it disrupts agricultural production and displaces people, leaving them without regular access to food, shelter or water. Food is sometimes weaponized during conflicts, leading to blockades or destruction of food supplies, which causes malnutrition to spike among civilians.
This can be seen in Sudan, where more than half of the population are now facing crisis or worse levels of food insecurity, forcing families to make impossible decisions to feed their children.
“The conflict in Sudan has decimated agricultural production, restricted the transportation of food, collapsed the banking sector, undermined local markets, and created large-scale displacement, all of which are limiting people’s ability to feed themselves,” said Eatizaz Yousif, the IRC’s Country Director for Sudan. “At the same time, restrictions on humanitarian access have severely limited humanitarian actors’ ability to reach populations in need.”
In Gaza, the escalation of hostilities in late 2023 created an unprecedented food crisis with the entire population of 2.2 million people facing high levels of acute food insecurity—the highest share ever classified for any area or country.
This crisis is being further exacerbated by recent U.S. aid cuts, which are severely impacting global malnutrition treatment programs. These cuts are forcing critical nutrition programs to scale back or shut down completely in vulnerable communities where humanitarian assistance is a lifeline. The impacts are particularly devastating for children who rely on peanut paste and pregnant and lactating women who face increased risks of maternal and infant mortality due to inadequate nutrition. Local health systems, already strained, are struggling to meet growing needs with diminished resources.
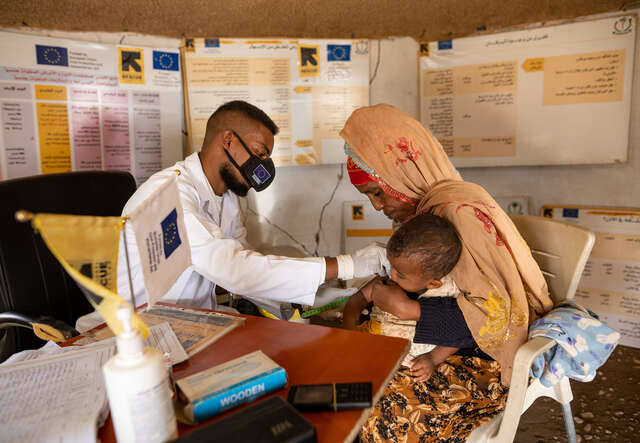
Why are children in need not receiving treatment?
Even though treatment for acute malnutrition is readily available, historically fewer than 1 in 5 children have received this life-saving care. The status quo approach to delivering care to malnourished children is complex, overly-bureaucratic and hobbled by a lack of sustained funding.
“With climate change and conflict exacerbating the global hunger crisis, it is more important than ever that we scale up simplified approaches to tackle acute malnutrition,” said Mesfin Teklu Tessema, Senior Director of Health at the IRC.
Malnourished children who need life-saving treatment are artificially divided into two groups: moderately and severely malnourished. Each is treated with different products, at different delivery points, supported by two different UN agencies — limiting the number of children that can be reached with finite resources.
Chronic underfunding remains one of the most critical barriers to addressing global malnutrition, and recent cuts to U.S. humanitarian aid have created an even more dire situation. These cuts threaten to unravel decades of progress in the fight against hunger and malnutrition, with consequences that extend far beyond immediate health impacts. As funding disappears, economies weaken through lost productivity, healthcare systems strain under mounting costs, and desperate families are forced to migrate in search of basic nutrition assistance. These budget decisions are quite literally matters of life and death for millions of vulnerable people, particularly children.
How does the IRC address acute malnutrition?
The IRC has been researching simplified approaches for treatment of acute malnutrition for a decade and the body of research is now significant. The evidence is consistent that simplified approaches are more cost-effective ways to treat acute malnutrition. The solution is a simplified treatment to reach every child.
The Movement against Malnutrition advocates for and champions all radically simpler, scalable and cost-efficient treatment approaches for acute malnutrition - and implements them in affected countries worldwide.
How does the IRC deliver treatment for malnutrition?
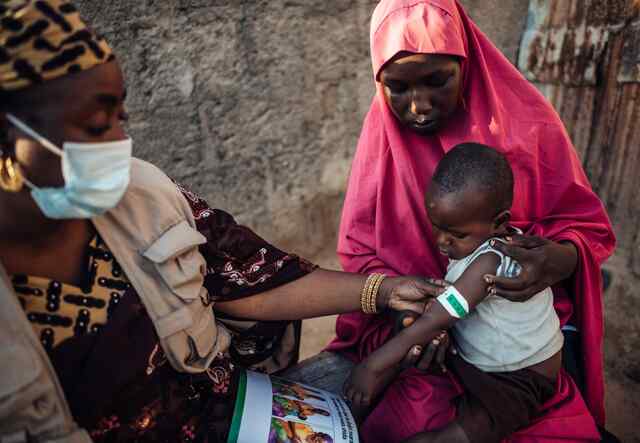
The IRC is leading innovation on simplified approaches to treating acute malnutrition, and ensuring more children receive life-saving treatment with the same resources, including treating all forms of acute malnutrition with a single food product at a single point of care, leveraging community health workers already embedded in local communities, and using simplified diagnosis and dosing.
“We are trying to reach mothers and children who are facing malnutrition so that we can provide them with health services and educational trainings,” says Agha, an IRC community health care worker in Afghanistan. “We want to raise awareness and guide them to care for their own health and prevent malnutrition in the future.
How effective is the IRC's approach?
The IRC has seen firsthand the impact simplified approaches can have in ensuring no child dies of hunger.
Evidence proves that simplified approaches are reliably and consistently effective. An IRC study in 2022, conducted in partnership with the Mali Ministry of Health, looked at more than 27,000 children treated for acute malnutrition with a simplified approach. 92 percent recovered in just weeks. The simplified approach also costs 20% less per child treated and uses 25% less product than the traditional protocol.
How can we treat more children experiencing acute malnutrition?
Our mission is to ensure no child dies of acute malnutrition. We plan to unify groundbreaking innovation, research, program delivery and advocacy to end this unconscionable global tragedy once and for all.
The Movement against Malnutrition advocates for and champions all radically simpler, scalable and cost-efficient treatment approaches for acute malnutrition - and implements them in affected countries worldwide.
“There are many horrific problems in the world for which we don’t have proven and scalable solutions, but treatment of acute malnutrition is not one of them,” said Amit Paley, the Executive Director of the IRC’s Movement Against Malnutrition. “The global community must take urgent action to save the lives of millions of children who need this simple, life-saving treatment now.”
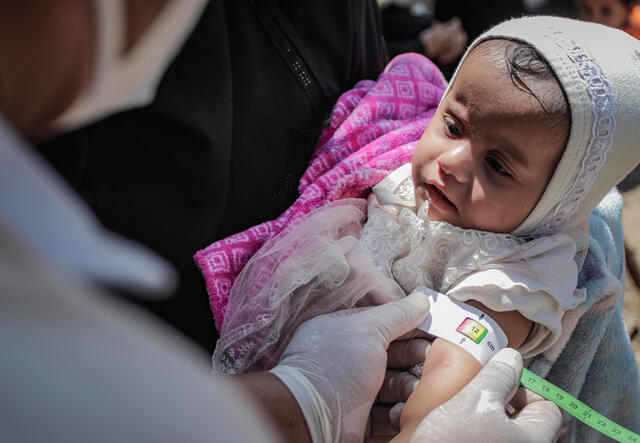
How can I help stop acute malnutrition?
Although a proven treatment for malnutrition is available, simplified approaches and funding to sustain them at scale are needed to treat the estimated 45 million children experiencing acute malnutrition around the world.
Donate to the IRC to help us address this and other crises around the world.
*Some last names excluded for privacy.



