
Over 5 million people have lost their lives to COVID-19. As Omicron and other COVID-19 variants continue to spread, our best defense is to vaccinate as many people as possible globally. Yet, millions in low-income countries and conflict zones continue to be ignored as wealthy nations prioritize boosters over equitable access to lifesaving vaccines.
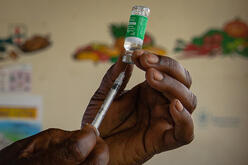
What this looks like in numbers:
Some 94% of people in low-income countries remain unvaccinated against COVID-19. Refugees and displaced people in countries affected by conflict and humanitarian crisis are especially vulnerable as variants spread.
Eight out of ten countries on the International Rescue Committee’s 2021 Emergency Watchlist are still less than 5% vaccinated, with the lowest coverage in:
- Democratic Republic of Congo - 0.06%
- Yemen - 1.16%
- South Sudan - 1.17%.
These countries could find themselves battling another COVID-19 variant without sufficient vaccine coverage to protect their populations.
Meanwhile, wealthier countries have now vaccinated the majority of their own populations, including:
- United States - nearly 58%
- United Kingdom - nearly 68%
- Germany - nearly 68%
- Sweden - nearly 70%
These four nations are starting to give booster shots while people in low-income countries go entirely unprotected.

COVID-19 vaccine inequality is particularly pronounced in Africa, which has received just 2.8% of the world’s vaccine doses, despite being home to 17% of the global population. The outlook is especially grim in the countries of the Sahel region, where ongoing violence has left millions of people in need of humanitarian assistance. Last month, for example, Burkina Faso saw a 31% increase in COVID deaths while Niger saw 22%.
Given limited access to testing, this is likely just the tip of the iceberg.
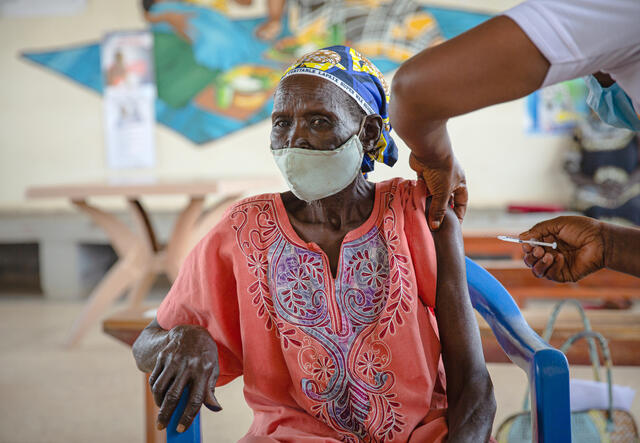
Health systems in countries that are affected by conflict and crisis are already overwhelmed. To save lives, COVID-19 vaccine donations from wealthier countries must be accompanied by sufficient funds to support vaccine delivery, diagnosis, and patient care.
“The race between vaccines and the variants is being lost in poorer countries while richer countries debate vaccine hesitancy,” says IRC president and CEO David Miliband. “This is dangerous as well as immoral. We are long overdue in rushing billions of vaccines as well as the funds to deliver them to frontline providers especially for last-mile delivery—and therefore into arms—in low-income and fragile contexts.”
The race between vaccines and the variants is being lost in poorer countries while richer countries debate vaccine hesitancy.
The U.S., U.K., Germany and Sweden have pledged vaccine doses to COVAX, the global initiative to ensure equitable access to COVID-19 vaccines for all countries. However, only 13% of promised doses have been delivered—and the world needs far more doses than what has been committed by donor nations.
Without additional vaccine doses and support for frontline health workers, Miliband explains, “new variants will only continue to undermine pandemic control globally—with the world’s most vulnerable paying the highest price.”

The Independent Panel for Pandemic Preparedness and Response called for 1 billion redistributed vaccine doses by September 1. To date, one quarter of that amount has been delivered to the poorest countries. The IRC urges high-income countries to increase their investments in COVAX and expand humanitarian funding and support for frontline responders.
The spread of Omicron globally is a concerning example of why the world needs to end vaccine inequality and scale up delivery to all, especially the most vulnerable.
How the IRC responds to COVID-19

The IRC’s global response to the COVID-19 pandemic focuses on preventing and responding to the spread of COVID-19 within vulnerable communities and working to meet immediate health and economic needs. We are also delivering COVID-19 vaccinations to refugees and displaced people in Uganda, Kenya, Somalia, Sierra Leone, Nigeria, Bangladesh, Pakistan, Jordan and other countries where we work.