
Many refugee and displaced women have gone through their pregnancies with no regular check-ups by midwives, no 12-week scans, no prenatal classes... They’ve faced war and persecution, survived in camps during the winter—and now they have the COVID-19 pandemic to worry about.
In places like northeast Syria and Bangladesh facing humanitarian crises, COVID-19 has stretched already strained health systems to their limits. As hospitals fill up with coronavirus patients, maternity services risk being squeezed, leaving pregnant women and their newborn babies without adequate care.
Our teams of committed midwives and doctors are going to the toughest-to-reach places to be there for women, during their pregnancy and beyond. Here’s how we help at every stage.
In the first nine months...
Our mobile health clinics in Yemen, drive to remote locations where families have found refuge away from war to provide critical care to pregnant women. Often, these expectant mothers would not have any other access to medical help. Yemen is on the brink of a famine, so providing enough food and nutrients is a crucial part of the support.
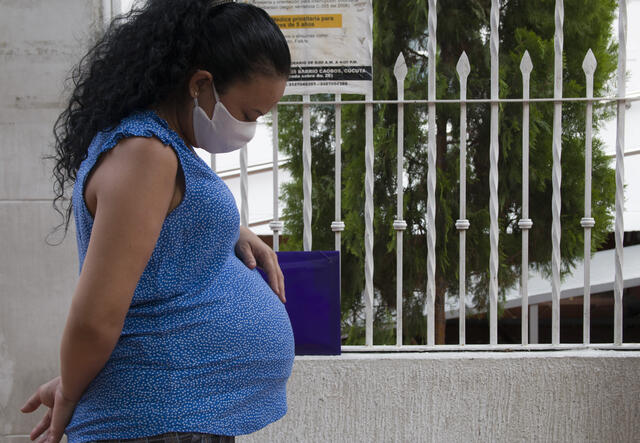
We’re also supporting pregnant women in Colombia who have fled violence and extreme poverty in neighboring Venezuela. Our center, which provides pre- and post-natal care, as well as family planning services and treatment for sexually transmitted infections, is right at the border. To ensure we’re keeping women safe during the pandemic, we’ve implemented social distancing and temperature checks, and have made sure staff have appropriate protective gear.
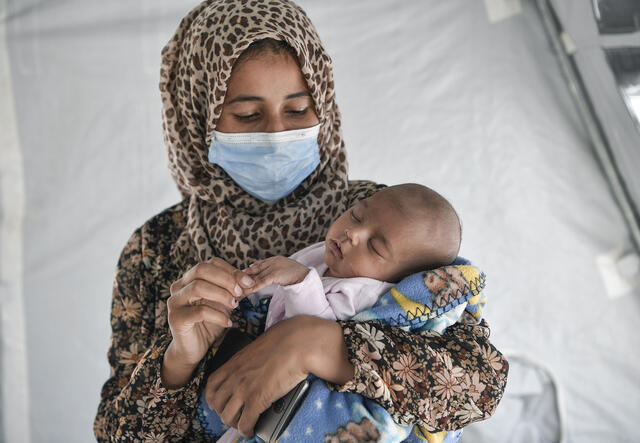
The threat of COVID-19 can make an already stressful situation even more difficult for refugee women about to give birth. In refugee camps, coronavirus testing is rare and misinformation about the virus spreads rapidly. We provide soap and water to families and have trained volunteers to go tent-to-tent in camps in Greece and Bangladesh, to ensure that women have the information they need to protect themselves during their pregnancy.
At the birth...
Following lessons learned in the Ebola crisis, the IRC has adapted our programs for another virus, COVID-19—creating isolation centers and providing protective clothing to ensure we can continue to deliver babies safely.
It’s essential that maternity services stay open during the COVID-19 pandemic. In Sierra Leone, researchers found that clinic closures and reduced reproductive health care services during the Ebola epidemic led to as many as 4,900 deaths of mothers and babies between 2014 and 2015.
Last month, in Dadaab refugee camp in Kenya, we helped a first-time mother, who had tested positive for COVID-19, deliver her daughter safely. Twenty-two-year-old Aamiina*, from Somalia, came to the IRC clinic with respiratory problems and was quickly given a COVID test. She was treated for her COVID symptoms but after 12 hours, had not progressed far enough in her labor. The team made the decision to conduct a C-section. Dressed in full protective gear, the IRC’s Dr. Lilian Mumbua operated successfully and both mother and baby are doing well.
Aamiina is just one of many women who have given birth during the pandemic with our support. Their strength and resilience are a daily inspiration for our frontline teams around the world.
In babies' first few months...

New mothers living in camps in places like northeast Syria and Greece, are doing all they can to make sure their newborns stay warm while living in tents. As another winter begins, this is going to get even tougher. We’re supporting mothers with newborn baby kits, which have items like blankets, diapers and baby clothes inside.
Um Tamer* has been displaced several times within her home country of Syria with her five children, including baby Zainab. Her pregnancy was incredibly difficult. “When I was pregnant, I was so stressed all the time, it was freezing. In the beginning, it didn’t sink in that we’re in a camp and that we have to live here.”

The IRC provided Um Tamer with a baby kit with essentials she needed to take care of her daughter. “When you have a newborn, things are expensive,” Um Tamer explains. “I was given the kit when she was five months old, it came at a really good time. Everything in it is useful: the clothes keep her warm because they have long sleeves, the diapers are important... I would advise other mothers in the camp to protect their newborns as much as possible from the cold.”
As mothers look to the future…
We’re giving parents the tools to ensure their children remain healthy as they go through life. Every year, 50 million children across the world suffer from acute malnutrition, and 80% of them are unable to access care. After four years of research, the IRC has developed a groundbreaking new way of treating acute malnutrition.

The treatment has helped support mothers like Binta, who was terrified when her 10-month-old son Ali started vomiting and had a fever. Like thousands of other families in northeast Nigeria, Binta had no income to pay for a doctor or pharmacy after armed groups forced her out from her village. Our clinic provides free care to children so they can recover from acute malnutrition. Parents like Binta now have the knowledge and expert medical support to keep their babies safe and healthy.
“I’m so relieved," Binta says of her son's recovery. "Because of the IRC, he’s back to normal.”
Learn more about the IRC's COVID-19 response over the past year.
*Names changed for protection
A version of this story was first published by IRC-UK.